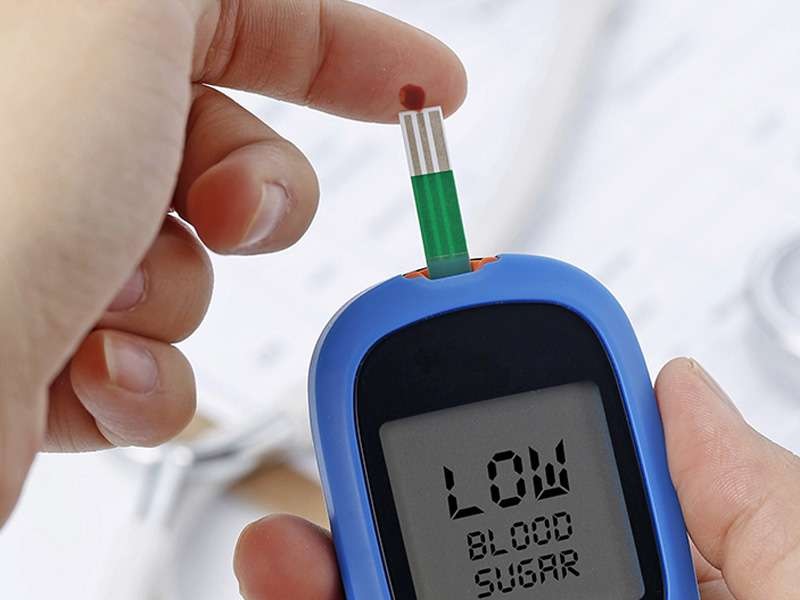
Diabetes is a chronic illness that affects millions of people worldwide. It is characterized by high levels of glucose (sugar) in the blood due to the body’s inability to produce enough insulin or use it effectively. Diabetes management involves various lifestyle changes, including diet, exercise, and medication. However, sleep is often overlooked as a critical factor in blood sugar regulation and overall diabetes management.
The Link Between Sleep and Blood Sugar Regulation
Studies have shown that sleep plays a crucial role in regulating blood sugar levels. Lack of sleep or poor sleep quality can lead to insulin resistance, which means that the body’s cells cannot use insulin effectively. This, in turn, causes glucose to accumulate in the bloodstream, leading to high blood sugar levels. Over time, this can contribute to the development of type 2 diabetes.
Moreover, sleep deprivation can also lead to an increase in stress hormones such as cortisol, which can further elevate blood sugar levels. This can be particularly problematic for people with diabetes, as they already have difficulty regulating their blood sugar levels.
The Importance of Sleep in Diabetes Management
Getting enough sleep is essential for overall health and well-being, but it is particularly important for people with diabetes. Adequate sleep can help improve insulin sensitivity and reduce the risk of developing type 2 diabetes. It can also help people with diabetes better manage their blood sugar levels and reduce the risk of complications such as heart disease and nerve damage.
Furthermore, sleep can also have a positive impact on other aspects of diabetes management. For example, getting enough sleep can help reduce stress levels, which can be beneficial for people with diabetes who may experience stress-related fluctuations in blood sugar levels. It can also help improve mood and cognitive function, which can help with diabetes self-management.
Tips for Improving Sleep Quality
If you have diabetes, it is essential to prioritize sleep as part of your overall diabetes management plan. Here are some tips for improving sleep quality:
- Establish a consistent sleep schedule and stick to it, even on weekends.
- Create a relaxing bedtime routine, such as taking a warm bath or reading a book.
- Avoid caffeine and alcohol before bedtime.
- Make sure your sleeping environment is comfortable and conducive to sleep, such as keeping the room cool and dark.
- Avoid using electronic devices such as smartphones or tablets before bedtime, as the blue light can disrupt sleep.
Sleep is a crucial yet often overlooked factor in blood sugar regulation and overall diabetes management. Lack of sleep or poor sleep quality can contribute to insulin resistance and high blood sugar levels, which can increase the risk of developing type 2 diabetes and its complications. Prioritizing sleep as part of a comprehensive diabetes management plan can help improve blood sugar control and reduce the risk of complications.